|
|
Hirsutism in Women
 Hirsutism
is defined as the presence of excessive terminal hair in
androgen-dependent areas of a woman's body. The disorder is a sign of
increased androgen action on hair follicles, from increased
circulating levels of androgens (endogenous or exogenous) or increased
sensitivity of hair follicles to normal levels of circulating
androgens. Hirsutism
is defined as the presence of excessive terminal hair in
androgen-dependent areas of a woman's body. The disorder is a sign of
increased androgen action on hair follicles, from increased
circulating levels of androgens (endogenous or exogenous) or increased
sensitivity of hair follicles to normal levels of circulating
androgens.
Hirsutism can develop at any age,
but most patients begin experiencing symptoms during their childbearing years.
In young girls who have not yet reached puberty, hirsutism is serious and could
be a sign of a hormone-secreting tumor. During
menopause, hirsutism is characterized by the thinning of underarm and pubic
hair with gradual hair growth in other parts of the body. In post-menopausal
women, sudden or severe hirsutism could be caused by an androgen-secreting
tumor.
Hirsutism
is a sign of increased androgen action on hair follicles, from increased
circulating levels of androgens or increased sensitivity of hair follicles
to normal levels of circulating androgens.
|
Commonly affected sites are the
face , neck, extremities, trunk, breasts, linea alba, lower back, upper pubic
triangle, and upper inner thighs . Unwanted hair is coarse, long and, often,
pigmented.
|
|
|
Type
|
Hirsutism can be either
androgen-dependent or nonandrogen-dependent (Drug-induced hirsutism).
Androgen-dependent Hirsutism
-
Hirsutism is caused by the
overproduction of androgens, which are the hormones responsible for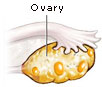 masculine qualities in either sex. While all women normally have some facial
hair, hirsutism is characterized by excessive or rapidly growing hair in
traditionally male areas of the body. If hirsutism is accompanied by other
symptoms such as acne, amenorrhea, deepening of
the voice, increased muscle mass or loss of breast tissue, this may signal a
hormonal abnormality. Androgen-excess syndrome has several major features:
seborrhea, acne, hirsutism,
alopecia,
obesity, and acanthosis nigricans. When
hirsutism is associated with obesity and menstrual abnormalities, the source
of androgen excess is often ovarian, typically polycystic ovary syndrome. When
it is associated with average weight and normal menses, the source is often
adrenal and rarely (in <5% of cases) pituitary.
masculine qualities in either sex. While all women normally have some facial
hair, hirsutism is characterized by excessive or rapidly growing hair in
traditionally male areas of the body. If hirsutism is accompanied by other
symptoms such as acne, amenorrhea, deepening of
the voice, increased muscle mass or loss of breast tissue, this may signal a
hormonal abnormality. Androgen-excess syndrome has several major features:
seborrhea, acne, hirsutism,
alopecia,
obesity, and acanthosis nigricans. When
hirsutism is associated with obesity and menstrual abnormalities, the source
of androgen excess is often ovarian, typically polycystic ovary syndrome. When
it is associated with average weight and normal menses, the source is often
adrenal and rarely (in <5% of cases) pituitary.
-
Decreased androgen binding in
the circulation - only free androgen is biologically active. Estrogens
increase liver manufacture of SHBG. Androgens decrease it. Thus lack of
estrogens can effectively increase available blood androgens. Also any
ingestion of androgens by mouth will further decrease SHBG and make those
ingested androgens even more available to stimulate hair growth.
-
Altered androgen metabolism
(conversion from weak to potent androgens) -
this is the most common cause of hirsutism and it appears to be the result
of an increased conversion in the skin of testosterone to DHT.
Nonandrogen-dependent (Drug-induced
hirsutism)
Many drugs can induce
hirsutism, both generalized and localized. These agents, too, are divided into
those that have androgenic activity and those that have nonandrogenic activity .
 Commonly used
drugs
that have androgenic activity are testosterone, dehydroepiandrosterone
sulfate (DHEAS), danazol (Danocrine), corticotropin, high-dose corticosteroids,
metyrapone (Metopirone), phenothiazine derivatives, anabolic steroids,
androgenic progestin, and acetazolamide (Dazamide, Diamox). Commonly used
drugs
that have androgenic activity are testosterone, dehydroepiandrosterone
sulfate (DHEAS), danazol (Danocrine), corticotropin, high-dose corticosteroids,
metyrapone (Metopirone), phenothiazine derivatives, anabolic steroids,
androgenic progestin, and acetazolamide (Dazamide, Diamox).
Common nonandrogenic drugs
that can cause hirsutism include cyclosporine (Neoral, Sandimmune, SangCya),
phenytoin (Dilantin), diazoxide (Hyperstat IV), triamterene-hydrochlorothiazide
(Dyazide, Maxzide), minoxidil (Loniten, Rogaine), hexachlorobenzene,
penicillamine (Cuprimine, Depen), and psoralens.
|
|
Hirsutism
can present with a broad spectrum of symptoms including the following:
-
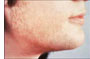 Excessive hair
growth - individuals with hirsutism will often present with excess hair on
areas of the body where hair follicles are sensitive to androgens including:
face, chest, breast, lower back, midline region of the lower abdomen, inner
thigh, arms, legs, etc. Excessive hair
growth - individuals with hirsutism will often present with excess hair on
areas of the body where hair follicles are sensitive to androgens including:
face, chest, breast, lower back, midline region of the lower abdomen, inner
thigh, arms, legs, etc.
-
Acne - excess androgen
associated with hirsutism can also contribute to the development of acne,
which may occur on the face, chest and/or upper-back.
-
Irregular menstrual cycle -
increased androgen levels can also disrupt the normal menstrual cycles. In
severe cases may cause women to be anovulatory.
-
Some major presenting complaints
may occasionally include: nipple discharge, emotional dysfunction, recurrent
miscarriage rate, pelvic pains
|
 Doctors
usually order blood levels of testosterone, to check out an ovarian
source and DHEA-S to check out an adrenal source of excess androgens.
If both studies show levels in normal range, treatment is directed
toward reducing the available androgens in blood circulation. Doctors
usually order blood levels of testosterone, to check out an ovarian
source and DHEA-S to check out an adrenal source of excess androgens.
If both studies show levels in normal range, treatment is directed
toward reducing the available androgens in blood circulation.
Two other hormonal tests,
prolactin and 17-OH progesterone may also be ordered especially if the
excess hair growth has been present since puberty, there is a strong family
history of hirsutism, ethnic background is Ashkenazi Jewish, a woman is
shorter than other family members or there is evidence of defeminization
such as a decrease in breast size. These risk factors can be associated with
genetic causes of adrenal hirsutism that do not always result in elevated
DHEA-S levels.
|
|
Treatment options for patients who
have hirsutism can be divided into
-
Measures targeting local
manifestations of hirsutism and
-
pharmacologic therapy aimed at
the underlying causes.
Therapy that targets local
manifestations includes physical methods of hair removal ranging from shaving to
laser therapy, topical treatment, and weight loss.
Measures targeting local
manifestations of hirsutism
Local measures such as
shaving, bleaching,
depilatories, and
electrolysis may be
used for hair removal. Shaving is the easiest and safest method, but is often unacceptable to patients.
Bleaching products are often ineffective for dark hair growth, and may cause
skin irritation . Chemical depilatories produce results similar to shaving, but
skin irritation is common. Electrolysis is one of the most effective and
permanent methods of hair removal, and may be an adjunct to hormonal treatment.
However, electrolysis is costly and time consuming, and has been replaced
by use of laser techniques.
Shaving is the easiest and safest method, but is often unacceptable to patients.
Bleaching products are often ineffective for dark hair growth, and may cause
skin irritation . Chemical depilatories produce results similar to shaving, but
skin irritation is common. Electrolysis is one of the most effective and
permanent methods of hair removal, and may be an adjunct to hormonal treatment.
However, electrolysis is costly and time consuming, and has been replaced
by use of laser techniques.
 The need
for rapid methods of hair removal has led to the development of
laser therapy for hirsutism. Several different lasers exist, including ruby,
alexandrite, pulsed diode, and Q-switched yttrium-aluminum-garnet (YAG) lasers.
Pulsed diode lasers are generally less expensive and more reliable than other
laser sources for hair removal. Q-switched YAG lasers work well in patients with
darker skin; however, these lasers are ineffective for long-term hair removal.
Most patients experience a two- to six-month growth delay after a single
treatment, and some have permanent hair removal after multiple treatments. Laser
therapy works best on dark hair. The need
for rapid methods of hair removal has led to the development of
laser therapy for hirsutism. Several different lasers exist, including ruby,
alexandrite, pulsed diode, and Q-switched yttrium-aluminum-garnet (YAG) lasers.
Pulsed diode lasers are generally less expensive and more reliable than other
laser sources for hair removal. Q-switched YAG lasers work well in patients with
darker skin; however, these lasers are ineffective for long-term hair removal.
Most patients experience a two- to six-month growth delay after a single
treatment, and some have permanent hair removal after multiple treatments. Laser
therapy works best on dark hair.
Each of these methods has
associated pros and cons which any consumer should consider. Temporary methods
which remove hairs by the roots (waxing, sugaring, threading) are considered
risky by some professionals due to the possible induction of bacteria into the
blood stream. Sanitary procedures should always be followed to avoid infection.
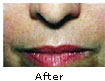
Vaniqa - is a new FDA approved prescription medication applied to the skin
for the reduction of unwanted facial hair. Vaniqa is prescribed for the treatment of unwanted facial hair
around the lips and under the chin. The fragrance-free medication is applied
similar to a moisturizing cream twice a day.
facial hair. Vaniqa is prescribed for the treatment of unwanted facial hair
around the lips and under the chin. The fragrance-free medication is applied
similar to a moisturizing cream twice a day.
Vaniqa works by actively inhibiting an enzyme located in the root of the hair
follicle, which is responsible for hair growth. The medical breakthrough, Vaniqa,
is proven to stop and prevent the growth of unwanted facial hair.
Note: If permanent hair
removal is your goal, do not purchase equipment or services that do not have
clearance unless you personally know someone who has had successful results. Ask
the manufacturer to mail you a copy of their 510(k) clearance letter from the
FDA or to supply you with their 510(k) number so you can look it up at the
FDA website
|
Pharmacologic
Treatment
|
Pharmacologic treatment
for hirsutism should be aimed at blocking androgen action at hair
follicles or suppression of androgen production
|
Medications Commonly Used in the Treatment of Hirsutism
Class of drug
|
Drug
|
Dosage
|
side effect and
warning *
|
Comments
|
Cost (generic)�
|
Oral contraceptives
|
Ethinyl estradiol with norgestimate,
desogestrel, norethindrone, ethynodiol diacetate
|
One tablet per day for 21 days, followed
byseven-day pill- free interval
|
GI distress, breast tenderness, headache,
intolerance tocontact lenses
|
Pregnancy category X No FDA labeling for
treatment of hirsutism
Least androgenic progestin component preferred
|
$31.00 per month
|
|
Ethinyl estradiol with drospirenone
|
|
Hyperkalemia may occur.
Contraindicated with hepatic dysfunction, renal insufficiency, adrenal
disease
|
Monitor serum potassium during first cycle
with concurrent use of NSAIDs, ACE inhibitors, angiotensin-II receptor
blockers, heparin, potassium supplements, potassium sparing diuretics.
|
29.00 per month
|
Antiandrogens (no FDA labeling for
treatment of hirsutism)
|
Spironolactone (Aldactone)
|
50 to 200 mg per day
|
Hyperkalemia (rare), theoretic
feminization of male fetus, gynecomastia
|
Pregnancy category D
Irregular bleeding may occur, monitor electrolytes.
|
29.00 per month (22.00 to 25.00)
|
|
Flutamide (Eulexin)
|
250 mg two to three times daily
|
Monitor liver function.
|
Combine with other method of
contraception.
Pregnancy category D
|
144.00 per month (125.00)
|
|
Finasteride (Proscar)
|
5 mg daily
|
Monitor liver function.
|
Pregnancy category X
|
70.00 per month
|
Glucocorticoids (no FDA labeling for
treatment of hirsutism)
|
Dexamethasone
|
0.5 mg nightly
|
Weight gain, hypokalemia, decreased bone
density, immune suppression
|
Pregnancy category C. May be combined with
oral contraceptives or Gn-RH agonists for severe hirsutism.
|
20.00 per month (2.00 to 10.00)
|
|
Prednisone
|
5 to 10 mg daily
|
|
Pregnancy category C
|
1.50 per month (2.00 to 3.00)
|
Gn-RH agonists (no FDA labeling for
treatment of hirsutism)
|
Leuprolide (Lupron)
|
3.75 mg IM per month for up to six months
|
Hot flushes, decreased bone mineral
density, atrophic vaginitis
|
Pregnancy category X. Use with caution for
short periods because of hypoestrogenic effect.
|
535.00 per month
|
|
|
11.25 mg IM every three months (depot
form)
|
May need add-back HT.
|
Use nonhormonal contraception during
treatment.
|
1,605.00 for three months
|
Antifungal agents (no FDA labelingfor
treatment of hirsutism)
|
Ketoconazole (Nizoral)
|
400 mg daily
|
Scalp hair loss, dry skin, abdominal pain,
fatigue, headache, vaginal spotting, hepatotoxicity
|
Pregnancy category C Use as last resort.
|
231.00 per month (182.00 to 190.00)
|
|
|
|
Monitoring of hepatic function necessary
|
|
|
Topical hair growthretardant
|
Eflornithine HCI(Vaniqa)
|
Apply to face twice daily at least eight
hours apart.
|
Skin adverse effects include acne,
erythema, stinging/burning, dry skin.
FDA approval for reduction of unwanted facial hair
|
Pregnancy category C
May cause mild elevations in transaminase levels.
No significant drug interaction known
|
42.00 for 30-g tube
|
Insulin-sensitizing agents (not FDA
approved for treatment of hirsutism)
|
Metformin (Glucophage)
|
500 mg twice daily 1,000 mg twicedaily (maximaldosage
2.0 to 2.5 g per day)`
850 mg three times daily
|
GI distress, lactic acidosis (rare with
mortality nearly 50 percent), numerous drug interactions
Monitor liver function, confirm normal renal function before
starting,and monitor.
|
Pregnancy category B
Resumption of ovulation may occur.
No FDA labeling for treatment of PCOS
|
47.00 per month (42.00)
|
GI =
gastrointestinal;
FDA = U.S. Food and Drug Administration;
NSAIDs = nonsteroidal anti-inflammatory drugs;
ACE = angiotensin-converting enzyme;
Gn-RH = gonadotropin-releasing hormone;
IM = intramuscular;
HT = hormone therapy;
PCOS = polycystic ovary syndrome.
*--For more detailed
information, consult the package insert provided by the manufacturer of each
drug.
�--Estimated cost to the
pharmacies (rounded to the nearest dollar) based on average wholesale prices
in Red book, Montvale, N.J.: Medical Economics Data, 2002. Cost to the
patient will be higher, depending on prescription filling fee.
Related Links
|
|
|
|
|





 Hirsutism
is defined as the presence of excessive terminal hair in
androgen-dependent areas of a woman's body. The disorder is a sign of
increased androgen action on hair follicles, from increased
circulating levels of androgens (endogenous or exogenous) or increased
sensitivity of hair follicles to normal levels of circulating
androgens.
Hirsutism
is defined as the presence of excessive terminal hair in
androgen-dependent areas of a woman's body. The disorder is a sign of
increased androgen action on hair follicles, from increased
circulating levels of androgens (endogenous or exogenous) or increased
sensitivity of hair follicles to normal levels of circulating
androgens. masculine qualities in either sex. While all women normally have some facial
hair, hirsutism is characterized by excessive or rapidly growing hair in
traditionally male areas of the body. If hirsutism is accompanied by other
symptoms such as
masculine qualities in either sex. While all women normally have some facial
hair, hirsutism is characterized by excessive or rapidly growing hair in
traditionally male areas of the body. If hirsutism is accompanied by other
symptoms such as  Commonly used
drugs
that have androgenic activity are testosterone, dehydroepiandrosterone
sulfate (DHEAS), danazol (Danocrine), corticotropin, high-dose corticosteroids,
metyrapone (Metopirone), phenothiazine derivatives, anabolic steroids,
androgenic progestin, and acetazolamide (Dazamide, Diamox).
Commonly used
drugs
that have androgenic activity are testosterone, dehydroepiandrosterone
sulfate (DHEAS), danazol (Danocrine), corticotropin, high-dose corticosteroids,
metyrapone (Metopirone), phenothiazine derivatives, anabolic steroids,
androgenic progestin, and acetazolamide (Dazamide, Diamox).
 Excessive hair
growth - individuals with hirsutism will often present with excess hair on
areas of the body where hair follicles are sensitive to androgens including:
face, chest, breast, lower back, midline region of the lower abdomen, inner
thigh, arms, legs, etc.
Excessive hair
growth - individuals with hirsutism will often present with excess hair on
areas of the body where hair follicles are sensitive to androgens including:
face, chest, breast, lower back, midline region of the lower abdomen, inner
thigh, arms, legs, etc.  Shaving is the easiest and safest method, but is often unacceptable to patients.
Bleaching products are often ineffective for dark hair growth, and may cause
skin irritation . Chemical depilatories produce results similar to shaving, but
skin irritation is common. Electrolysis is one of the most effective and
permanent methods of hair removal, and may be an adjunct to hormonal treatment.
However, electrolysis is costly and time consuming, and has been replaced
by use of laser techniques.
Shaving is the easiest and safest method, but is often unacceptable to patients.
Bleaching products are often ineffective for dark hair growth, and may cause
skin irritation . Chemical depilatories produce results similar to shaving, but
skin irritation is common. Electrolysis is one of the most effective and
permanent methods of hair removal, and may be an adjunct to hormonal treatment.
However, electrolysis is costly and time consuming, and has been replaced
by use of laser techniques.  The need
for rapid methods of hair removal has led to the development of
The need
for rapid methods of hair removal has led to the development of

